Email us:
info@andrea-digestive-clinic.comCall us:
+65 6264-2836#21-11/12 Royal Square Medical Centre
Mon - Fri : 9am - 5pm, Sat : 9am - 1pm
Colonoscopy screening is a procedure that enables your doctor to examine the lining of the rectum and colon. It is performed in the endoscopy suite at the medical centre or hospital of your choice.
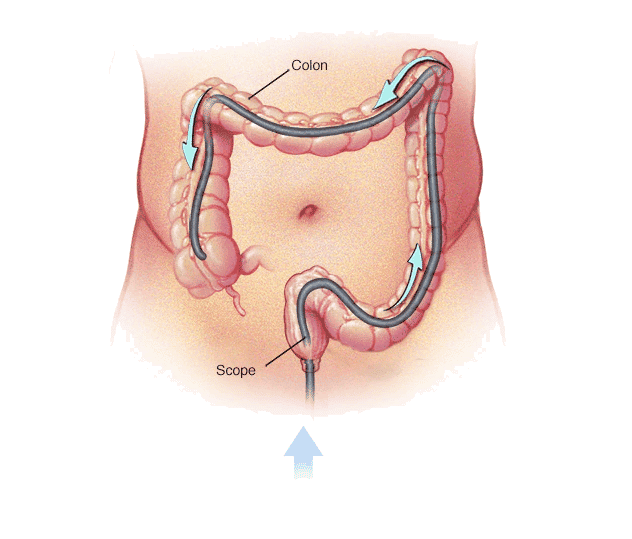
A soft, flexible tube about the thickness of a finger is gently inserted into the anus and advanced through the rectum and colon. The tube has a built-in camera that allows your doctor to see the interior of your colon, checking for polyps, signs of colon cancer or colorectal cancer and tumours, or other abnormalities.
As our bodies change as we age, it is suggested that persons over the age of 50 years of age schedule yearly examinations with their gastroenterologist or doctor to ensure continued good health of the gut. Should the need arise (such as unexplained weight loss, or if the doctor suspects colorectal cancer or colon cancer), the doctor or gastroenterologist will recommend a colonoscopy. Colon cancer and colorectal cancer rank highly among cancer deaths in Singapore, in persons over 50 years old.
Colonoscopy is performed for conditions such as:


The colon must be completely emptied of stool for the procedure. In general, this involves bowel cleansing, prior to the screening colonoscopy. You will be given instructions on the bowel preparation.
Bowel preparation can involve taking a liquid called PEG or laxatives followed by water to clean out the bowel.
If you are unable to complete the preparation, it may not be possible to perform the colonoscopy and the procedure will be postponed.
Most medications are safe to continue before the procedure. Please inform your doctor before the examination, especially if you are taking any blood thinners warfarin, aspirin or diabetes medication.

In Singapore, the patient is given sedation during the colonoscopy to minimize any discomfort. During sedation, the doctor will slowly advance a colonoscope through the colon to examine its lining. The procedure is usually completed in 20 to 30 minutes depending on the complexity of the individual procedure.
After the procedure, some recovery time is usually allowed to let the sedative wear off. Outpatient recovery time can take an estimate of 30–60 minutes. The patient is allowed to take a light meal before discharge. A common after effect from the procedure is a bout of flatulence and occasionally minor wind discomfort caused by air insufflation into the colon during the procedure.
For colonoscopy in Singapore, the price can vary greatly depending on the types of procedures involved, where it is done and the doctor’s fee. At our clinic, we offer cost counselling services for our patients. Please enquire with us to find out more about cost counselling and how we can help you further.

Colonoscopy is a very safe procedure. Complications are rare, but can occur. These include bleeding (<1%) and bowel perforation (0.2%). Bleeding can occur up to about 2 weeks after a colonoscopy. Rarely surgical treatment is needed. Some patients might have reactions to the sedation.
It is important to contact your doctor if you experience symptoms of severe abdominal pain, fever or rectal bleeding after colonoscopy.

You will be observed until the sedation has worn off, after which you will be discharged home. Do not drive or operate machinery till the next day, as the sedatives used will impair your reflexes.
You may experience mild cramping or bloating from the air placed in the colon. This will improve quickly when you pass gas. You will be able to eat normally the same day and resume your normal activities the next day. If you feel persistent pain or develop a fever or experience bleeding when passing motion, do not hesitate to give your doctor a call to check on whether the situation is normal.
